Jambo!
We’ve got another full day at the clinic planned with Continuing Medical Education in the morning and patients in the afternoon. We’ve reserved today for following up with patients who are currently in the Chronic Disease Program.
The topics for the CME include:
- Dr. Michael: Brucellosis
- Dr. Tanya: Dyspepsia, GERD and Peptic Ulcers
- Dr. Tanya: Tips for Physical Examination
Dr. Michael’s talk involved Brucellosis, an infectious disease caused by a type of bacteria called Brucella which can spread from animals to humans. There are several different strains of Brucella bacteria, but the main ones found in Lewa’s herding community are the ones found in cattle, goats and sheep. People contract the bacteria by eating or drinking unpasteurized dairy products by animals infected with the Brucella bacteria. In terms of symptoms, fever by itself is a big telltale sign. Once other conditions like malaria are ruled out, a test can be done which will confirm the diagnosis.
We’ve determined that the clinic has been treating the patients with the correct medication but for a shorter duration than is recommended. It is a difficult condition to cure and recurrence is common. Therefore following the longer treatment schedule is really important. In fact, 20% to 30% involve the bones and joints, often resulting in back pain. This is called osteoarticular disease and is treated with the same medication but with a longer treatment plan.
Later in the morning, Dr. Tanya provided a clinical training session on how to conduct a proper abdominal examination. Our nurse Kristen bravely volunteered to be the “patient” so that Dr. Tanya could demonstrate the techniques and the clinic staff could practice. It was a fun and easy atmosphere with lots of laughing, which I think resulted in a very safe environment for learning. The staff asked lots of questions and demonstrated their knowledge giving Dr. Tanya an opportunity to offer tips and guidance. She would pose questions like, “If you want to examine the spleen, where would you press? How would you go about it?” or “How do you test for an enlarged liver?” It proved so useful that we decided to try to fit in a session on cardiovascular clinical assessment before we leave.

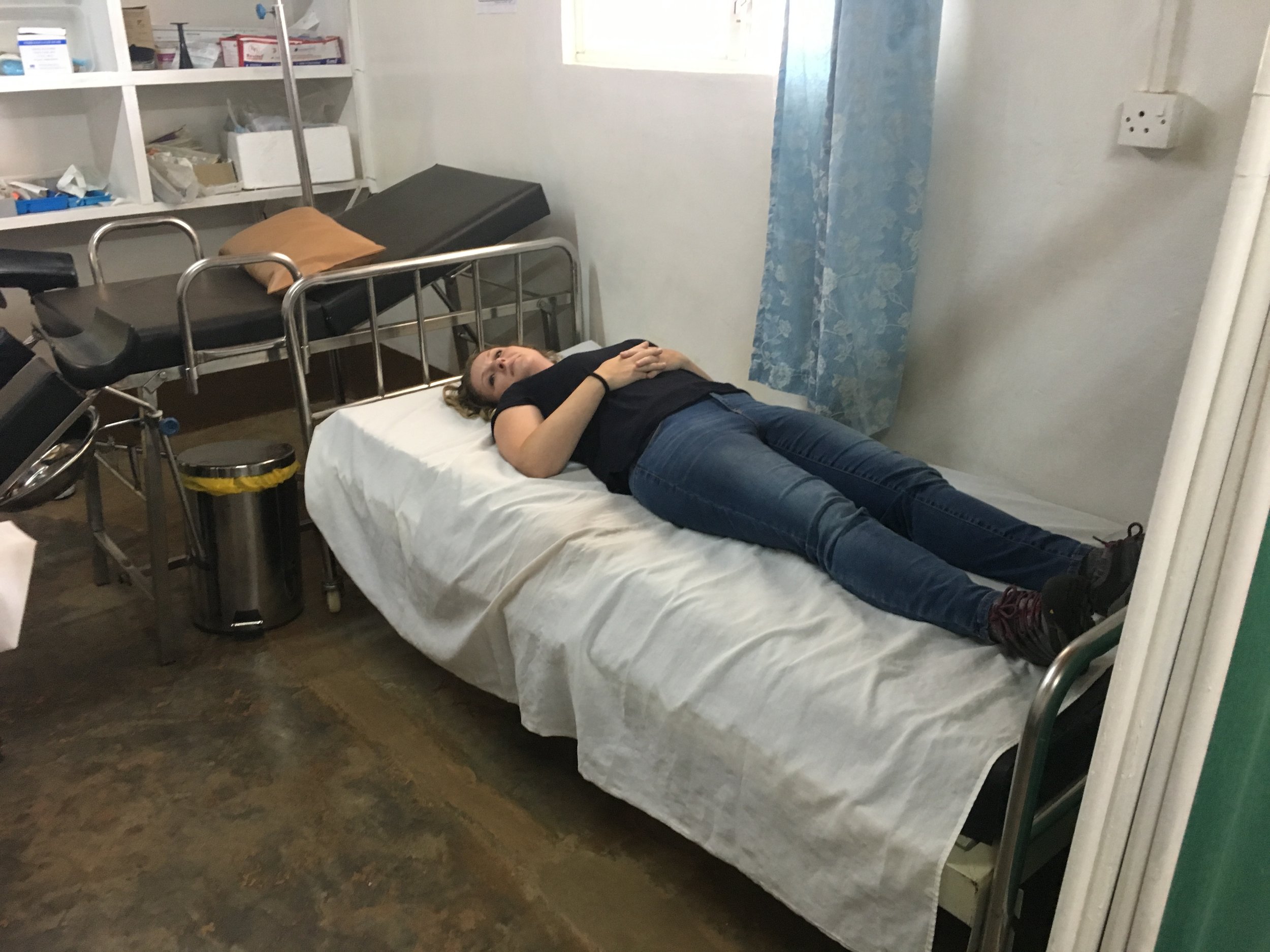

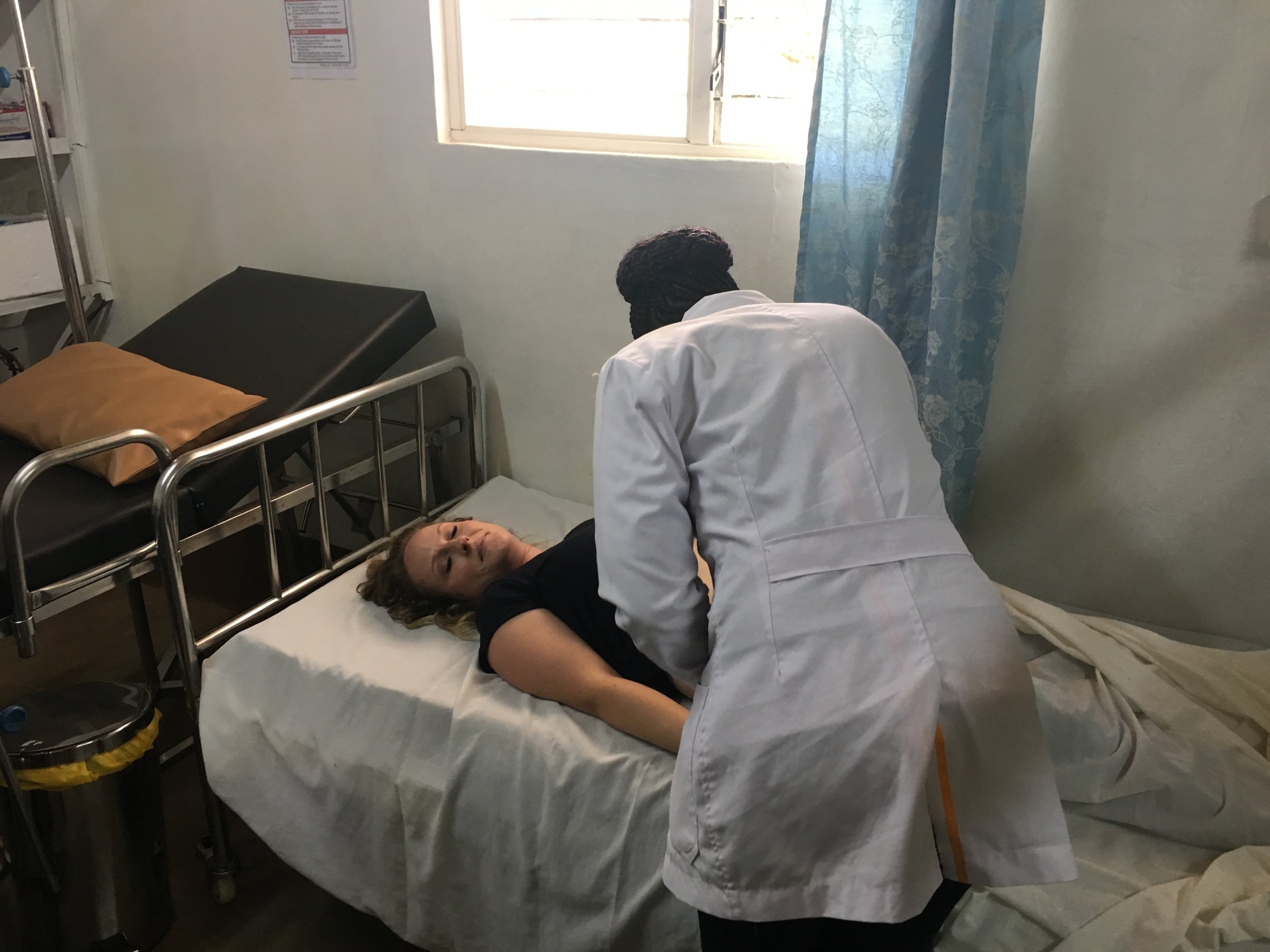
After lunch we headed back to the clinic to see our chronic disease patients. Dr. Tanya’s first patient is a gentleman who has had a stroke. Before the actual stroke, he went in to the hospital after falling when he got up in the middle of the night to use the washroom. He arrived at the hospital presenting with stroke-like symptoms. But the hospital sent him home after observing him for several hours and the initial symptoms disappeared. Dr. Tanya said to the staff that this was unfortunate as this scenario suggests that what the man had experienced was a “mini stroke” or transient ischemic attack (TIA) and that it should have been a big sign to the hospital that he was at very high risk of having a stroke. And sadly, the next day, he had a stroke and is dealing with some paralysis on his right side. The paralysis will likely not improve, but he’s able to walk very slowly with a cane.
This case was an excellent opportunity for Dr. Tanya to ask lots of questions of the nurses with regard to his current treatment plan. They identified that his blood pressure was still too high and that they should adjust the dosage to bring it within the protocol limits. We then discover it is not easy to determine what medications the patient is taking. The medication that is listed in his file seems to be inconsistent with what the man (and his wife) thinks he takes. We’ve advised him to bring in all of his medication next time so that they can confirm that he is taking the right drugs and the correct dose. Unfortunately, inconsistencies in the information you receive from patients is very common and can be a challenge when trying to care for them. Our doctors remind me this is true everywhere in the world and is not just the case here in Kenya. Poor record keeping can also layer on another obstacle to ensuring this patient is prescribed the correct medication. The EMR that we’re building will help with this immensely. Each patient will have an electronic file which we can use to manage the patient in terms of their prescriptions, dosages, reminders for follow-up visits, etc.
Dr. Michael and Jen had a meeting with Phoebe to review the Chronic Disease Program, including the list of eligible patients as well as the drugs that we will cover. Some of our challenges have been ensuring only those patients screened by Emily (our CHW) will be included in the program and that only the chronic disease drugs that we approve will be covered by Naweza. It is simply growing pains and we’re hoping through clear guidelines and lots of communication any potential issues will be mitigated.
Dr. Sidiqa visited the Naweza-sponsored optometrist who comes to the clinic once a month to provide training to Lydia, conduct vision tests and write prescriptions if necessary. On our last trip, we planned for Lydia to do vision screening at a school of 500 students. Any of the students who failed the test would be directed to the clinic to be followed up with the optometrist. He would examine the student and write a prescription for glasses. Naweza would pay for these glasses. However, we noticed that there weren’t any prescriptions written and we were wondering why. He indicated that the problem was that transportation to the clinic was too difficult for the children, so the kids weren’t able to have their follow-up assessment. We didn’t realize this would be an issue when planning this pilot project. Now the plan is to have Naweza pay for transportation and hopefully the children will soon have their glasses!
Our sponsored optometrist's clinic
The optometrist also indicated that other people who come in for the monthly vision clinics don’t want to pay for the glasses and so he hasn’t been writing any prescriptions. However, through working with suppliers, Naweza has obtained a much lower price ($10-16 per pair versus $50 per pair). We thought our optometrist was aware of this discounted price, and it’s not actually clear where the breakdown in communication occurred, but it’s a reminder to us the importance of constant communication and touching base just to see how the project is coming along. The plan now will be to revisit these patients and offer them the better price and hopefully provide them with their glasses.
Tomorrow will be our outreach day. We’ll be heading to Ngare Ndare, the same location as the last time we were here. It will be great to see the community again and hopefully provide some help to them. It will be our chance to connect with hundreds of patients and create goodwill with the people. It is truly one of our favourite days, despite the chaos that inevitably ensues! But I’m sure with Rosaline there, all will be just fine!
Until tomorrow, lala salama!
Stacy ☺





